There’s good news for many Veterans receiving prescriptions from VA. As of February 27, 2017, the regulations for copayments will change. The cost to most Veterans for medications required on an outpatient basis to treat non-service connected conditions will be less. Most Veterans will see a $1 to $4 savings per prescription filled. Some Veterans may see a small ($2 to $3) increase for brand name (called “Tier 3”) outpatient medications. Additionally, Veterans in priority groups 2 – 6 will see a decrease in their annual copayment cap of $960 go down to $700 a year while Veterans in priority groups 7 and 8, who currently don’t have an annual cap, will see a $700 cap per year as well.
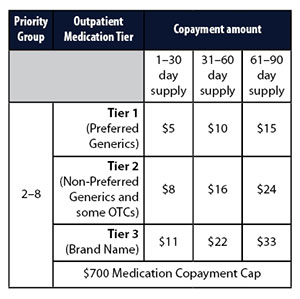
Copayments Based On Tiers
Veterans who are currently exempt from copayments will continue to be exempt. Veterans with a large number of outpatient medication copayments will save even more. VA does not charge Veterans a premium, similar to what health insurance companies expect, so their only out-of-pocket costs will be the copayments. VA’s goal is to reduce out-of-pocket costs and simplify getting prescriptions to Veterans. This will also benefit Veterans in rural communities, where VA medical centers and local pharmacies may not be close to the Veterans home.
